Coordinating the COVID-19 Research Response

April 28 Update: For those helping to 3D print headbands for face shields: please be sure you are using the latest version (V4.2).
Note: This is not an exhaustive list of COVID-19 research efforts affiliated with Virginia Tech. In immediate response to the COVID-19 pandemic, Virginia Tech faculty, staff, and students have initiated numerous research projects in an effort to support the local community and to affect humanity on a global scale.
Read: Virginia Tech community converges to help meet need for COVID-19 medical supplies.
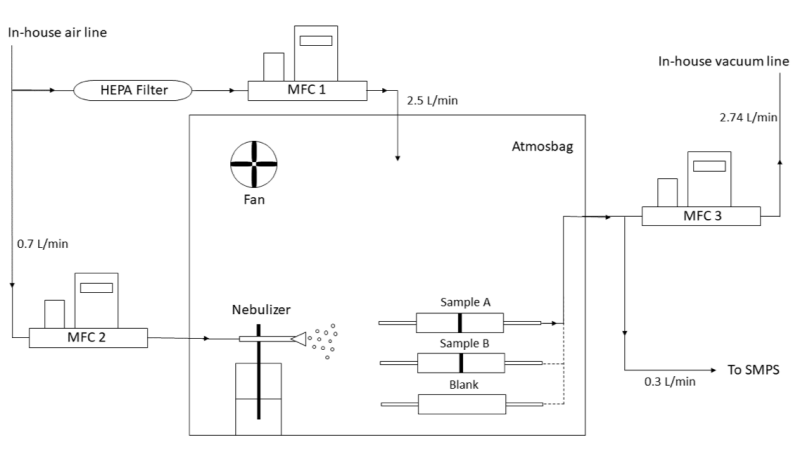
Dr. Linsey Marr's lab has the unique capability to evaluate filtration efficiency of porous media down to 0.02 microns — sufficient for validating the 95% filtration standard for N95 masks. These tests are ongoing.
Dr. Matthew Hull is leading efforts at ICTAS to a) help healthcare providers secure certified PPE through ProjectN95, b) identify decontamination solutions for re-use of PPE, c) develop a retrofit solution for creating powered air-purifying respirators (PAPRs) from widely available surgical togas, d) create and support a NRV/Roanoke regional outreach initiative to acquire medical fabrics and assemble them into masks for first responders and essential employees, and d) coordinate acquisition of alternative viral barrier materials for evaluation and use in VT-developed PPE/medical device prototypes.

Project Leads
- Linsey Marr, Charles P. Lunsford Professor, Civil and Environmental Engineering (lmarr@vt.edu)
- Matthew Hull, Business Development Manager, ICTAS (mahull@vt.edu)
Face shields are an essential piece of PPE to protect health care workers from patient sneezing or coughing. However, face shields are a quickly dwindling resource across hospitals.
More than 2,000 face shields have already been manufactured and delivered. At the current rate, Virginia Tech is producing around 700 face shields per week.
This team evaluated several open-source designs and then underwent several rounds of feedback with New River Valley providers. This feedback resulted in a modified design that features a 3D printed headband and laser cut transparent plastic sheet with full face coverage. The face shields can be reused following sterilization via wiping or alcohol submersion, and have been approved for use by the hospital's infection control department.
The Virginia Tech full face shield can be found on the NIH 3D Print Exchange.



The project lead, Dr. Alex Leonessa (faceshields@vt.edu), is actively soliciting contributions for bulk filament, bulk elastic, and bulk sheets of polyester. In particular polyester is out of stock almost everywhere and difficult to secure. Any availability for 3D printing time would be greatly appreciated as well.
For details on how to contribute to the production of full face shields, please click the link below.
April 28 Update: For those helping to 3D print headbands: please be sure you are using the latest version (V4.2).
Project Lead
- Alex Leonessa, Professor, Mechanical Engineering (faceshields@vt.edu)
Another idea from our Carilion colleagues is to use an ambu bag mask, with a HEPA virus filter attached, to serve as reusable PPE. However, this novel design doesn't fit under existing face shields. The Virginia Tech team is designing a face shield that will conform to the protruding HEPA virus filter. The solution will include 3D printed headbands paired with laser cut plastic film that conforms around the mask and filter.

Project Lead
- Liam Chapin, Lab Manager in Dr. Erik Komendera's FASER Lab (wchapin@vt.edu)
Virginia Tech faculty are working with pulmonology experts to create an approach for converting BiPAP machines into low-level respirators. In addition to adding HEPA filters to the circuit to protect caregivers, this novel approach includes designing and fabricating an in-line, bi-directional flow meter to verify and calibrate flow to and from the patient, as well as designing and programming a data acquisition system for automated flow monitoring. The flow meter will have adjustable alarm limits to notify nurses and doctors if the patient is not receiving the appropriate amount of flow.

Project Lead
- Joseph Meadows, Assistant Professor, Mechanical Engineering (jwm84@vt.edu)
A makeshift adapter device for a BiPAP conversion idea was created to connect a readily available filter to the exhalation port in order to prevent virus particles from being blown out into the room at the caregivers. However, the adapter required components taken from two separate sterilized kits, and the remaining valuable kit components would be discarded.

To alleviate this, and to reduce the number of seams in the assembly, this project aims to fabricate hundreds of couplers that have similar airflow restrictions of the makeshift adapter and are also disposable. These couplers are fabricated through CNC turning of Delrin, and thanks to Techsburg in Christiansburg, 200 have already been delivered to Carilion for infection safety and regulatory review before production and public use.
The resultant face shield design can be found on the NIH 3D Print Exchange.
Project Leads
- Chris Williams, Professor, Mechanical Engineering (cbwill@vt.edu)
- Genevieve Gural, Graduate Student in Dr. Williams' DREAMS Lab (ggural@vt.edu)
There has been a great effort among scientists and engineers to design 3D printed face masks or other alternatives for N95 face masks; however, scientific evaluation is needed to validate their efficacy. Several masks from the leading open-source designs have been 3D printed and delivered to Dr. Linsey Marr's lab for testing. Masks were printed using multiple additive manufacturing processes and materials, including: desktop fused deposition modeling (ABS, PLA), industrial fused deposition modeling (ULTEM), and industrial selective laser sintering (nylon).
In addition to evaluating existing mask designs, the DREAMS lab is exploring alternate designs and processing routes, including a resuable design that can be rapidly manufactured with vacuum-forming from a 3D printed pattern. This design would be coupled with a silicone part to create a seal with the user's face and a 3D printed threaded filter holder.


Project Leads
- Chris Williams, Professor, Mechanical Engineering (cbwill@vt.edu)
- Genevieve Gural, Graduate Student in Dr. Williams' DREAMS Lab (ggural@vt.edu)
- Sam Pratt, Graduate Student in Dr. Williams' DREAMS Lab (pratts@vt.edu)
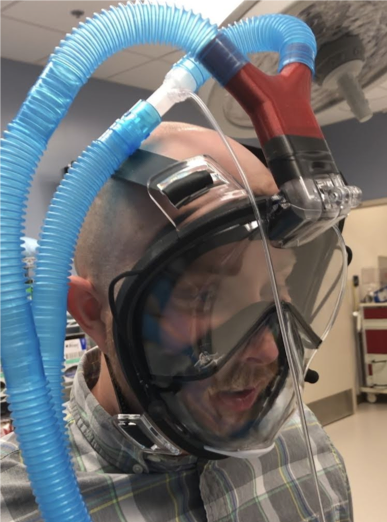
To further address the need for N95 masks and face shields, Virginia Tech is adapting off-the-shelf snorkel masks to make full-face passive respirators. This project develops connectors for four different mask models that can be fabricated by inverse stereolithography, a type of additive manufacturing (3D printing). The custom adaptors are required to connect the masks to various types of viral filters or pressurized air supplies. Testing of the assembled prototypes is underway in Dr. Linsey Marr’s lab. The project team is poised to produce up to 200 modified snorkel masks.

Project Lead
- Marc Michel, Associate Professor, Geosciences and Nanoscience (mfrede2@vt.edu)
Due to supply concerns, local doctors are in need of reusable (sterilizable) housings for respirator circuit HEPA filters. This project team is researching 3D printing of autoclavable materials (e.g., fused deposition modeling of ULTEM) to fabricate these requested parts.
The HEPA shell design feature a double ring and snap-together assembly. Once finalized, this team could potentially produce up to 200 shells per week.

Project Leads
- Chris Williams, Professor, Mechanical Engineering (cbwill@vt.edu)
- Logan Sturm, Graduate Student in Dr. Williams' DREAMS Lab (ldsturm@vt.edu)
In order to ramp up COVID-19 testing, Drs. Finkielstein and Michel are working to fabricate nasal swabs using inverse stereolithography 3D printing. Leveraging designs from the University of South Florida, the project team has demonstrated 3D printing capabilities at Virginia Tech, assessed the mechanical properties of the printed swabs, and established a lab on campus. At current capacity, the lab can produce around 650 swabs per day, and there is room for expansion if needed.
Project Leads
- Carla Finkielstein, Associate Professor, Biological Sciences (finkielc@vt.edu)
- Marc Michel, Associate Professor, Geosciences and Nanoscience (mfrede2@vt.edu)


